Prostate cancer … and PSA testing
Raising awareness of men’s health issues in Movember, and beyond
Did you know that prostate cancer is the most commonly diagnosed cancer in men in the UK, according to Prostate Cancer UK and Cancer Research UK, affecting 1 in 8 in their lifetime?
Currently, the Movember charity (supporting and raising awareness for men’s health) says there are ‘more than 395,000 men living with and beyond the disease in this country. Globally, more than 1.4 million men are diagnosed with prostate cancer each year.’
Every November, ZoomDoc supports the drive to raise awareness of prostate cancer – and other health issues primarily affecting men.
‘Knowing the warning signs to look out for is key all year round and we can’t stress enough the importance of talking to your GP as soon as you find something that doesn’t look or feel right,’ says ZoomDoc CEO, Dr Kenny Livingstone.
So read on to find out everything you need to know about this key cancer affecting men, including warning signs and symptoms and where to get help.
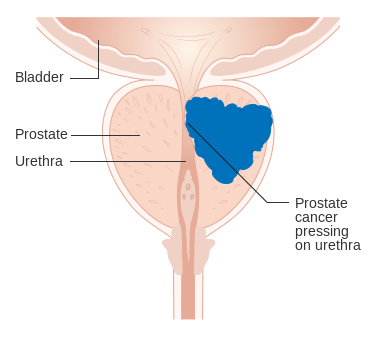
What exactly is prostate cancer?
Prostate cancer is the most common cancer in UK males, accounting for more than a quarter (27%) of male cases. Your chances of getting it increase with age, with most cases developing in men over the age of 50.
Prostate cancer affects the walnut-sized gland (the prostate) that sits just below the bladder and produces some of the fluid in semen. Although most cases develop slowly, with no noticeable signs for some years, some types are more aggressive and can spread quickly without treatment.

What are the warning signs of prostate cancer?
The nature of prostate cancer and the way it grows means you’re pretty unlikely to notice any early warning signs or symptoms.
However, the NHS says it’s always worth getting these symptoms checked out by a doctor:
- an increased need to pee
- straining while you pee
- a feeling that your bladder has not fully emptied.
These symptoms don’t necessarily mean you have prostate cancer but are worth getting checked as they can also be a sign of something called benign prostatic hyperplasia (BPH). Often confused with prostate cancer, this isn’t cancer and can be treated if required.
Once prostate cancer is more advanced, symptoms can include:
- back pain, hip pain or pelvis pain
- problems getting or keeping an erection
- blood in the urine or semen
- unexplained weight loss.
However, these symptoms can also be attributed to other health conditions, not just prostate cancer.
So, how do I know if I’ve got prostate cancer?
With very few early symptoms presenting themselves, nor any test you can do yourself, such as looking for lumps or physical changes, ‘knowing the risk factors and your family’s health history plays a big part,’ says Dr Kenny.
‘Your risk increases with age, mostly – although not always – affecting those over the age of 50.
Black men or men with a family history (a brother or father with prostate cancer) are more than twice as likely to get it, too,’ he adds
It’s a myth that too much sex, a vasectomy or masturbation can increase your chances of prostate cancer developing. If you have an enlarged prostate (BPH), that does not mean you are at greater risk of developing prostate cancer, either.
Getting tested for prostate cancer
There’s currently no single test or screening programme for prostate cancer in the UK. According to the NHS, ‘this is because it has not been proved that the benefits would outweigh the risks.’
If you are concerned about your risk or any unusual symptoms, your doctor may recommend:
- A digital rectal exam (DRE) to feel for bumps or hard spots on the prostate
- A blood test to measure prostate-specific antigen (PSA), a protein produced by prostate cells. (More on this below.)
- An MRI scan
- A biopsy.
How do PSA tests work?
PSA tests can help detect prostate cancer in its early stages although it isn’t fully conclusive and can create false-positives. Although an elevated level of PSA may indicate a higher chance that you have cancer, it’s also possible to have a high level and still be cancer-free. It is also possible to have a normal PSA and have prostate cancer.
Currently men over 50 can ask for a routine PSA test on the NHS. This can be available younger if you have a family history of prostate cancer.
Struggling to get an appointment?
Get a PSA home test with ZoomDoc Health
‘ZoomDoc provides simple home self-testing kits that enable you to monitor your PSA level at home, particularly helpful if you’re struggling to get an appointment with your GP or if you simply want to re-check and monitor your level’, says Dr Kenny.
This finger prick blood test analyses your (PSA) prostate specific antigen level, which may be elevated in prostate cancer, as well as a number of other benign conditions. The results are reliably analysed by our team of GPs.
Buy your self test PSA kit here.
What happens after you’ve taken ZoomDoc’s PSA home test?
A normal PSA level is considered to be under 4 nanograms per milliliter (ng/mL) of blood, while a PSA above 10 suggests a high risk of cancer.
But there are many exceptions:
- Men can have prostate cancer with a PSA less than 4.
- A prostate that is inflamed (prostatitis) or enlarged (BPH) can boost PSA levels, yet further testing may show no evidence of cancer.
- Some BPH drugs can lower PSA levels, despite the presence of prostate cancer, called a false negative.
If either a PSA or a digital rectal examination test are abnormal, your doctor will likely recommend other further tests.
These may include:
- a scan
- a biopsy or,
- a direct referral to a urology specialist.
Treatment for prostate cancer
If you are diagnosed with prostate cancer, it’s worth knowing that many prostate cancers are slow growing and may not need surgery or other radical treatment. The actual risk of dying from prostate cancer is around 3% – and many cases do not warrant treatment at all.
However, treatment options include:
- Active surveillance
- Prostatectomy
- Radiotherapy
- Hormone therapy
- Chemotherapy
If you need a referral to a specialist or further advice on prostate cancer, get in touch with our team of ZoomDoc doctors.

