When you’re full of the flu or just can’t shake that cough/cold, you’d probably do anything for a prescription to make you feel better. But after a trip to the doctor’s, who hasn’t felt disappointed when their GP says antibiotics aren’t the answer?
With concerns over antibiotic resistance, doctors these days are much more mindful of over prescribing them – and rightly so, says ZoomDoc’s Chief Medical Officer, Dr Kenny LIvingstone.
‘There’s no doubt that a bad cold or virus can make you feel really unwell, but most viruses really will get better on their own, with rest, fluids and time. It’s frustrating but antibiotics just won’t help – and taking them too often or when they’re not needed simply increases the risk of antibiotic resistance – where they don’t work when you really need them to,’ he says.
So what do antibiotics help with and how can you get a prescription when you really do need one? Here’s what you need to know …
What exactly are antibiotics?
‘Antibiotics are used to treat specific types of bacterial infection, by killing the bacteria and stopping it from spreading,’ says Dr Kenny.
Put simply, they kill the bacteria or prevent it from spreading further, but they don’t work for everything.
For instance, it is often not advised to use antibiotics for a cold, flu, or most coughs, as these tend to pass on their own. Antibiotics are also not used routinely for:
- Ear infections in children
- Sore throats
- Chest infections
There are lots of different types with some better at treating milder, more common infections (such as tonsillitis or ear infections, if required) and others better for serious illnesses (such as sepsis and meningitis.)
If you have been prescribed antibiotics, always follow your doctor’s advice on when to take them, and how long for. It is common to start feeling better and stop taking the antibiotics as a result. In doing this, though, you may see a relapse in the infection, and have to resume or start antibiotic treatment all over again.
Penicillin is one of the more commonly prescribed groups of antibiotics, although if you’re allergic to this kind then you’ll be recommended an alternative.
What can antibiotics treat?
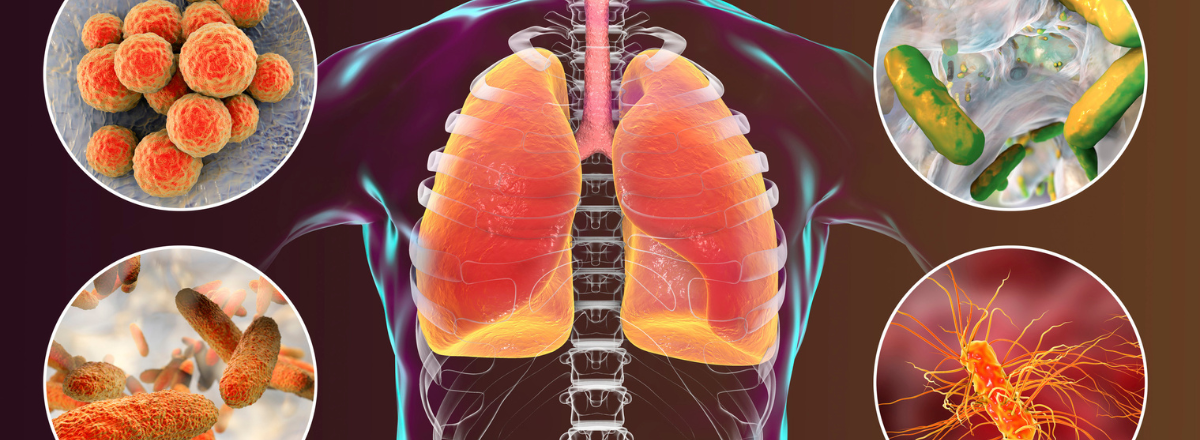
Antibiotics work by blocking vital processes in bacteria. They kill the bacteria or stop it from spreading.
‘Bacterial infections, not viruses’, says Dr Kenny. ‘Antibiotics are not effective against colds, coughs or viral infections, which are common at this time of year,’ he says.
They should only be used to treat serious or persistent bacterial infections that could spread easily, could cause complications or don’t get better, such as:
- acne
- cellulitis
- meningitis
- pneumonia
- impetigo
- sepsis
- sexually transmitted infections (STIs)
- eye infections
- animal bites or wounds.
They may also be used:
- Preventatively, for instance, before or after an operation to avoid infection to a wound, or ahead of labour if you test positive for Group B Strep, to prevent this being spread to your newborn baby.
- For health problems that aren’t serious, but can spread to other people. This could the likes of chlamydia, or impetigo.
- If evidence suggests that antibiotics could improve recovery speeds, for instance with kidney infection.
- Where more serious complications could occur, for instance with pneumonia or cellulitis.
If a course of antibiotics doesn’t work then your GP may prescribe an alternative antibiotic to try. Always finish the full course, even if you start feeling better.
Pros and cons of antibiotics

The overuse of antibiotics in recent years means they’re becoming less effective and has led to the emergence of “superbugs”.
There’s no doubt that antibiotics have the power to save lives – a huge pro. Other pros for antibiotics include:
- They can prevent infections before surgery.
- They are fast-acting.
- Most are easy to take.
- They can slow the growth of and kill many types of infections.
However, in order to remain that way, the NHS no longer recommends them for ‘routine use’ when treating infections, such as throat, ear and chest infections, instead reserving them for when they’re really needed.
Cons of antibiotics:
- many infections are caused by viruses, so antibiotics are not effective
- antibiotics are often unlikely to speed up the healing process and can cause side effects like sunlight sensitivity and bone damage.
- Antibiotics can impact the effectiveness of the contraceptive pill, so ensure you use extra protection while taking them.
- Long term use of antibiotics can cause damage to the body’s immune system.
Alongside these cons, the more antibiotics are used to treat trivial conditions, the more likely they are to become ineffective for treating more serious conditions. This is a part of the antibiotic resistance problem, and will likely become a major issue for the future of medicine.
‘Antibiotic resistance is a worldwide problem where overusing them in the past has made them less effective. A consequence of this is the emergence of superbugs, which simply don’t respond to antibiotics and can be fatal,’ says Dr Kenny.
And as with any medications, antibiotics carry the risk of side effects, such as nausea, rashes, drowsiness or breathing difficulties. Call your GP if you suffer any side effects or think you may be allergic to what you’ve been prescribed.
What types of antibiotics are there?
Antibiotics are generally broken down into 6 different classifications, although individually there are hundreds of different types of antibiotic. The different classifications are:
Penicillins
Penicillins are used to treat a great number of infections, from urinary tract infections, to chest infections and skin infections.
The penicillin classification includes penicillin, flucloxacillin, phenoxymethylpenicillin, and amoxicillin, and co-amoxiclav.
Penicillin is one of the more commonly prescribed groups of antibiotics, although if you’re allergic, you’ll be recommended an alternative.
Cephalosporins
Cephalosporins can be used to treat many types of infections, but are also proven in treating more serious infections like meningitis.
An example of a Cephalosporin might be cefalexin, which is most often used to treat issues like pneumonia, UTIs, and other chest infections.
Aminoglycosides
Aminoglycosides are largely only used for very serious illnesses like sepsis. They are mostly administered in a hospital because there are serious side effects attributed to them. Side effects may include kidney damage and loss of hearing.
Examples of aminoglycosides include gentamicin and tobramycin. These antibiotics are typically given by injection, although drops for ear and eye infections may also be administered.
Tetracyclines
Tetracyclines are used to treat a wide range of infections. Acne sufferers and rosacea sufferers typically use this antibiotic to manage any infections as a result of their conditions.
Examples of Tetracyclines include tetracycline, doxycycline, and lymecycline.
Macrolides
If you have a penicillin allergy, you may be given macrolides as an alternative. These antibiotics are users for a number of infections, including lung and chest infections, as well as infections that are resistant to penicillin.
Examples of Macrolides include azithromycin, erythromycin and clarithromycin.
Fluoroquinolones
These antibiotics were once used widely to treat a number of infection, in particular respiratory and urinary tract infections. They are no longer used as routine antibiotics now, as there is a risk of serious side effects.
Examples of Fluoroquinolones include ciprofloxacin and levofloxacin.
Alternatives to antibiotics

Ibuprofen is used to manage and treat inflammatory diseases, rheumatoid disorders, mild to moderate pain & fever.
If you’re feeling unwell and viral this winter, there are medicines you can use to alleviate symptoms and reduce fever or pain.
‘To help manage symptoms, take age-appropriate doses of paracetamol in a 24-hour period. If this doesn’t help you can alternate paracetamol doses with ibuprofen,’ says Dr Kenny.
Unfortunately there is no evidence that cough medicines or cough remedies work. The US is also considering banning the sales of over-the-counter decongestant products containing the ingredient phenylephrine, which studies show to be ineffective.
Getting a prescription for antibiotics

Order repeat prescriptions, and learn how pharmacists can help you with medicines and medical advice.
You can’t get antibiotics without a GP prescription, which you’ll need to pay for (unless you’re eligible for free prescriptions).
If you’re struggling to get a doctor’s appointment, call the practice and explain what you need. It’s possible the GP will need to see you, but if you need a repeat course of antibiotics or an alternative course, you may be able to get this arranged over the phone.
Alternatively, talk to a ZoomDoc GP via our app and one of our doctor’s will be able to assess whether you need antibiotics, or not. If you do then we can include a prescription as part of our service but you will still have to pay for it at the pharmacy, unless you have an exemption.
Do not be tempted to buy prescription medicine online, which could be counterfeit and highly unsafe.
Frequently Asked Questions around Antibiotics and Winter Bugs
[H3] Do antibiotics make you more susceptible to a cold?
Research from the Washington University School of Medicine suggests that antibiotics can make you more susceptible to colds. The research from an interview with Larissa Thackray on Livescience states:
“Some groups of bacteria are depleted, and different species grow out. It’s likely that antibiotic use could increase susceptibility to any virus that is controlled by T-cell immunity, and that’s many of them.”
Can overuse of antibiotics cause superbugs?
There is a great risk of superbugs emerging due to overuse of antibiotics. This is because antibiotics are often taken when they are not needed, and the more antibiotics that are used, the more likely a drug-resistant bacterium will emerge. There is also a risk of drug-resistance being shared with other bacteria. This could result in drug-resistant superbugs emerging that may be very dangerous.
What is the winter bug in the UK?
The winter bug in the UK is also known as the norovirus. This virus causes diarrhoea and vomiting, and contrary to popular belief, can be caught all year round. You would not be given antibiotics for norovirus. The only way to overcome it is to stay well hydrated, rest, and let it run its course.