We’re all guilty of overindulging at Christmas and putting on a few pounds thanks to mince pies, tubs of chocolates and festive pints. But most of us will manage to lose the weight we gain without needing much help or support.
But for one in four adults suffering from obesity in this country, the struggle to lose a few festive pounds, let alone the excess weight they’ve been carrying all year is real.
That’s why National Obesity Week (10-16 January) is kicking off 2024, working with the government, to raise awareness of the growing obesity problem in this country that currently costs the NHS an enormous £6.6 billion a year (source: gov.uk).
Tackling obesity head on will not only reduce pressure on hospitals, it’ll also boost the economy and save lives, possibly even your own.
So to kick off 2024, here’s why we all need to get behind obesity and make it a thing of the past, not a predicted part of our future.
What is obesity and why is it a problem?

In the UK it’s estimated that around 1 in every 4 adults and around 1 in every 5 children aged 10 to 11 are living with obesity.
If you’re obese you have excess body fat that makes you very overweight. You’ll have an unhealthy body mass index (BMI), a number that calculates a healthy weight for your height.
Calculate yours here.
Having a BMI that’s too high – over 30 – meaning you’re obese or severely obese, rather than a healthy weight or even overweight, is particularly bad for your health.
Obesity puts a strain on your heart, increasing your risk of heart disease as well as:
- diabetes
- certain cancers
- stroke
- high blood pressure
- indigestion
- sleep problems
- asthma
- pregnancy complications
- infertility
It can also be linked to mental health conditions such as depression.
What causes obesity?
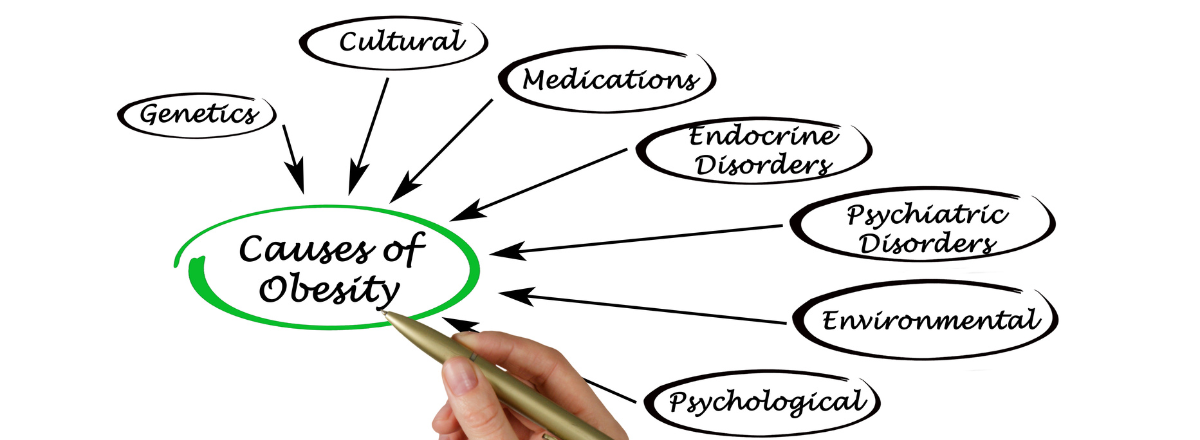
Obesity is a complex issue with many causes. It’s caused when extra calories are stored in the body as fat.
The NHS describes obesity as a ‘complex issue’. It can be caused by overeating fatty and calorific foods that don’t get burned off as fuel and instead are stored in and on the body as fat.
However, obesity can also be caused by:
- genetics
- thyroid conditions
- medications, such as steroids
- depression, which can lead to overeating.
How to get help for obesity
Obesity currently affects one in four adults (26%) and almost the same percentage (23.4%) of children aged 10-11 years. These numbers are placing a huge pressure on the NHS and on individuals’ life expectancy. Each generation has always outlived the generation before them, but the obesity crisis now means children will live shorter lives than their parents’ generation.
Fortunately, in many cases, obesity is preventable and while getting results can take willpower, self-motivation, hard work and support, help is at hand.
Diet and exercise help for obesity
Treatment for obesity will start with following a healthy, lower-calorie diet combined with regular exercise.
This will require willpower, self-motivation and patience as well as support, which can come from your GP, a dietitian or slimming group, such as Slimming World.
Exercise doesn’t have to be anything too rigorous but it does need to be regular. The NHS recommends walking, jogging or swimming for 2.5-5 hours a week, that’s roughly 30-60 minutes most days of the week.
Making realistic goals is key. You’re looking for a lifestyle change that is sustainable long-term so cutting all treats out and joining an intimidating gym isn’t necessarily the best place to start.
Try finding sensible food swaps or a diet that works for you that you’re likely to stick to. And save your money from gym memberships to stepping out on the pavement or working out in your lounge. You’ll see results and save money!
Joined a gym and need to cancel?
If you’re diagnosed with obesity and your gym membership isn’t working for you, order our Gym And Health Club Cancellation Certificate. For £40 we’ll provide you with evidence that you need to suspend or cancel your membership due to a medical condition (obesity or obesity-related illness). Of course, we highly recommend continuing some form of exercise with the guidance of your GP after cancellation.
What if diet and exercise doesn’t work?
If you’ve tried diet and exercise and still need help with losing weight, your GP may recommend the following, if they are suitable for you:
Orlistat – according to the NHS, ‘if taken correctly, this medicine works by reducing the amount of fat you absorb during digestion.’
Liraglutide – other medicines such as liraglutide or semaglutide (Wegovy, Ozempic) can work by making you feel fuller, less hungry and therefore helping you eat less.
Weight loss surgery – if you’ve tried other weight loss methods, surgery such as gastric bands or gastric bypass may be a long-term option.
Wegovy and Ozempic: what’s the difference?
The weight-loss jab semaglutide, known as Wegovy and Ozempic, has been found to improve blood sugar control and weight loss.
Semaglutide, mentioned above, is usually marketed by the more commonly used brand names of Ozempic or Wegovy.
Both are produced by Novo Nordisk, a Danish pharmaceutical company, but Ozempic contains 1mg of Semaglutide, compared to 2.4mg in Wegovy.
Aside from this, they work in much the same way, mimicking the action of a hormone called glucagon-like peptide-1 (GLP-1) that naturally occurs in the body and helps regulate blood sugar levels, suppresses appetite, and slows down digestion.
They both also help regulate blood glucose levels, which is especially beneficial for individuals with type-2 diabetes.
Neither should be used for more than two years continuously, and must be taken under the guidance of a doctor or specialist weight-loss team with regular monitoring.
Read more about semaglutide here.
Not getting the obesity support you need? Talk to our ZoomDoc GPs with an online appointment. Or order a same-day GP Referral letter and make an appointment to see an obesity specialist or dietitian privately.

