Obesity has reached epidemic proportions across the developed world, with serious implications for public health. The UK has one of the highest rates – according to the National Obesity Observatory, 63.4% of adults in the UK were overweight or obese in 2022. This is a significant increase from 1993, when only 48.1% of adults were overweight or obese and this figure is projected to rise further in the coming years.
The rise in obesity has been driven by a number of factors, including changes in diet, declining physical activity levels, and the availability of ultra-processed foods. This development has significant health implications, including cardiovascular disease, type 2 diabetes, stroke, dementia and certain types of cancer. Tackling obesity requires a multifaceted approach that encompasses lifestyle changes, dietary modifications, and, in some cases, medical intervention.
What is Semaglutide and how does it work for weight loss??
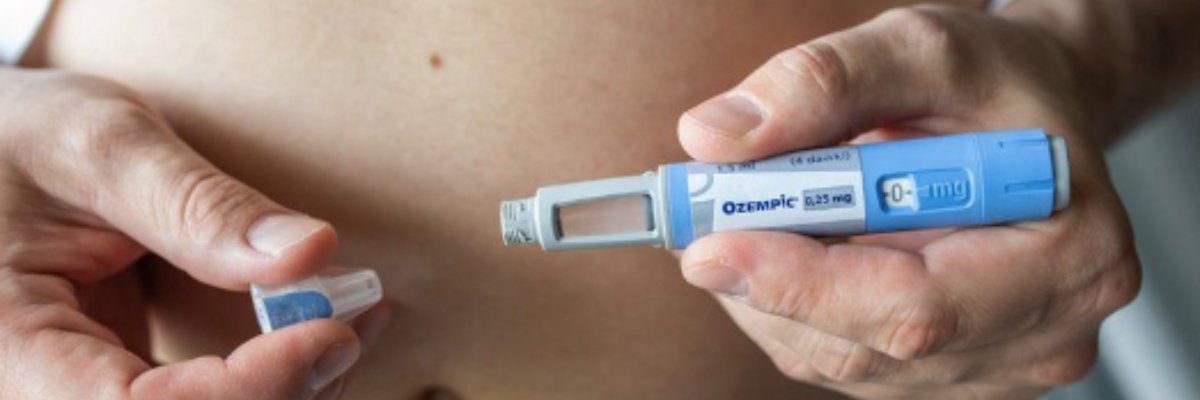
Semaglutide (Ozempic), is an antidiabetic medication used for the treatment of type 2 diabetes and an anti-obesity medication.
Semaglutide is a prescription medication, administered by weekly subcutaneous injection, that belongs to a class of drugs known as GLP-1 receptor agonists – originally licenced for type 2 diabetes. It has exploded in popularity since its regulatory approval for weight loss 2 years ago due to a combination of impressive study results and celebrity endorsements.
Semaglutide is usually marketed by the more commonly used brand names of Ozempic or Wegovy. They are both produced by Novo Nordisk, however Ozempic contains 1mg of Semaglutide, versus up to 2.4mg in Wegovy.
It works by mimicking the action of a hormone called glucagon-like peptide-1 (GLP-1) that naturally occurs in the body. GLP-1 helps regulate blood sugar levels, suppresses appetite, and slows down digestion. By activating GLP-1 receptors, Semaglutide helps control appetite, leading to reduced food intake and increased feelings of fullness. It also helps regulate blood glucose levels, which is especially beneficial for individuals with type 2 diabetes.
Semaglutide: The Evidence for Weight Loss.
A number of studies have been particularly exciting in demonstrating the effectiveness of Semaglutide for weight loss. One study, called the SUSTAIN 6 trial, found that people lost an average of 12.4% of their body weight over a period of 68 weeks1. This was significantly more than the people who took a placebo, who lost an average of 2.4% of their body weight.
Another study, called the SCALE trial, found that people who took Semaglutide lost an average of 14.9% of their body weight over a period of 56 weeks2. There was also the STEP5 trial, which was a larger, longer-term study that included over 15,000 people who were overweight or obese. The people who took Semaglutide lost an average of 10.2% of their body weight over a period of 168 weeks versus the placebo group, who lost an average of 2.4% of their body weight3.
In 2023, a new study was published that looked at the effectiveness of an oral version of Semaglutide – understandably many people would rather take a tablet than inject themselves! The study, called STEP 64 included over 3,000 people who were overweight or obese. In this, the people who took the oral version of Semaglutide lost an average of 10.6% of their body weight over a period of 56 weeks which makes it broadly comparable to the injectable version.
The results of these studies suggest that not only is the injectable version effective for weight loss, the oral version of Semaglutide appears to be comparably effective. However, it is important to note that these studies were relatively short-term, and this class of medication has only been in use for the last 15yrs. As such more research is needed to see what the safety profile of Semaglutide looks like over the long term.
Semaglutide: The Safety Profile.
The most common side effects of Semaglutide are nausea, vomiting, diarrhoea, and constipation. These side effects usually go away within a few weeks of starting treatment, however for a small number of people they do not. This was the main reason people stopped taking the medication in clinical studies. Other side effects that have been reported include headache, fatigue, and dizziness. In 2022, the European Medicines Agency (EMA) issued a warning about a possible increased risk of suicide with Semaglutide. Despite this, they concluded that the benefits of Ozempic still outweigh the risks for most people.
It is also important to note that due to the rapid weight loss, many people using Ozempic have reported a significant proportion of their weight loss has come from muscle rather body fat. This can have the perverse effect of increasing a person’s fat-to-muscle ratio and even putting some older individuals at higher risk of frailty. The risks of muscle loss are higher in those who are older, do little resistance training whilst taking Ozempic and had an inadequate protein intake. For similar reasons, Bone Mineral Density can be reduced increasing the risk of fractures, and some clinics require their patients to get this assessed through a DEXA scan prior to initiating treatment.
Semaglutide: Who Should Take It?

Technically, a patient is a candidate for semaglutide for weight loss purposes if their BMI is greater than 27
Semaglutide is not for everyone, however the criteria differ if it is being issued on the NHS or privately. It should only be taken by people who are overweight or obese and who have a BMI of 30 kg/m2 (35 within the NHS) or higher, or a BMI of 27 (30 within the NHS) or higher with a related health condition such as type 2 diabetes. The NHS does however use lower BMI thresholds (usually reduced by 2.5 kg/m2 ) for people from South Asian, Chinese, other Asian, Middle Eastern, Black African or African-Caribbean family backgrounds5.
Semaglutide should also not be taken by people who have a history of pancreatitis or who are pregnant or breastfeeding. Additionally it should not be used for more than 2 years continuously, and needs to be taken under the guidance of a doctor or specialist weight-loss team with regular monitoring.
Future developments

The NHS 12-week weight loss plan is designed to help you lose weight safely and keep it off, by sticking to a daily calorie allowance and getting active.
Semaglutide is just one of a number of new weight loss drugs that are being developed. Other drugs in this class include tirzepatide (Mounjaro) and dulaglutide (Trulicity) which work in a similar way to Semaglutide, by mimicking the action of GLP-1 and appear to be achieving good results in early clinical studies.
It is likely that we will see more of these drugs being developed in the future. As our understanding of obesity and its causes improves, we will be able to develop even more effective and safe weight loss treatments.
Conclusion
Semaglutide is a promising new weight loss drug that has been shown to be effective in clinical trials. However, it is important to note that it is not a miracle cure and it does have side effects. It is important to talk to your NHS GP – or one of our Zoomdoc medical team about whether Semaglutide is right for you.
Worryingly, due to its boom in popularity Semaglutide is now unavailable in many pharmacies across the country. This is causing many issues for those whose need is perhaps ‘more urgent’ such as those with type 2 diabetes, and are now struggling to access their prescribed medication.
Furthermore it’s important to remember that weight-loss is perfectly possible without medication. By adhering to (and sticking with) a diet that creates a daily calorie deficit and increasing your activity levels – ideally with an enjoyable sport, weight loss and its associated benefits are available to and achievable by all. Whatever your weight-loss ambitions, Zoomdoc are here to help.
References
- https://www.nejm.org/doi/full/10.1056/nejmoa1607141
- https://www.nejm.org/doi/full/10.1056/nejmoa1411892
- https://www.nature.com/articles/s41591-022-02026-4
- https://www.thelancet.com/journals/landia/article/PIIS2213-8587(22)00008-0/fulltext
- https://www.nice.org.uk/guidance/ta875/resources/semaglutide-for-managing-overweight-and-obesity-pdf-82613674831813

